What is Zika?
*See below for latest updates
Zika virus was discovered in Ugandan forests almost 70 years ago. There is currently active transmission in more than 40 countries in the Americas, the Caribbean, the south Pacific Islands, and in Cape Verde in Africa. This virus is transmitted primarily by the bites of infected mosquitoes, most commonly by Aedes aegypti. These mosquitoes are aggressive daytime biters (indoor and outdoor) but can also bite at night.
There is no vaccine to prevent infection and there is no medication that can treat it. The incubation period is unknown, but is likely a few days to a week. Most people who become infected have no symptoms but some may experience fever, skin rash, joint pains, muscle aches, headaches and red eyes. Treatment consists of rest, fluids and acetaminophen to reduce fever. NSAIDS (e.g. aspirin, ibuprofen, naproxen, should be avoided). Symptoms usually last a week and the person is likely immune after thereafter. Testing is performed by detection of the viral RNA in blood within 7 days of onset of illness and in urine up to 14 days after the onset of symptoms. It is important that anyone infected with the virus try to avoid being bitten by a mosquito within that first week, to prevent the mosquito becoming infected and transmitting the disease to another person.
Why is the Zika virus significant?
In February 2016 the WHO became very concerned about clusters of microcephaly in infants born to women who had been infected with Zika in pregnancy and Guillain-Barre syndrome (GBS) in adults in areas of Zika activity. On April 7, 2016 the WHO reported that there is scientific consensus that Zika infection is a cause of microcephaly and GBS. Microcephaly is a very small head and brain in a fetus and is associated with abnormal mental function. The virus may also cause other fetal brain and eye abnormalities as well as miscarriage in early pregnancy and fetal death. Women exposed to the virus can be followed by serial ultrasounds in pregnancy to look for microcephaly. Accuracy of ultrasound depends when it is performed in pregnancy, the severity of the microcephaly, ultrasound equipment used, and expertise of the person performing the test. GBS affects the nervous system of an adult and may cause paralysis, usually temporary.
How do I try to prevent being bitten by mosquitoes?
Measures to help prevent being bitten by mosquitoes include use of repellants (e.g. DEET, picardin, oil of lemon eucalyptus), wearing long sleeved shirts and long pants, staying in places with air conditioning, use of window and door screens, and sleeping under a mosquito net in areas of active transmission by mosquitoes. Picardin should not be applied to children under the age of 2 years and oil of eucalyptus should not be applied to children under the age of 3 years. DEET is the only repellant that has been at all investigated in pregnancy, and there were no harmful effects to the fetus when it was applied to the skin in 900 women during the second and third trimesters. Animal studies have shown no ill effects of DEET to a fetus when applied in any trimester.
How is Zika transmitted between people?
- An infected person may be bitten by a mosquito which may then bite another person and transmit the infection.
- Zika can be transmitted sexually by ejaculation of infected semen into the vagina, anus, or mouth of a female or male partner (fellatio).
- To date, there are no reports of Zika transmission from an infected female to a male through vaginal intercourse or oral sex (cunnilingus). The virus has been detected in saliva, urine and breast milk, but not in vaginal swabs collected from women with Zika.
- To date, there have been no reports of Zika being transmitted through kissing.
- Zika can be transmitted from a pregnant mother to her fetus via the placenta.
How many Zika infections in the U.S. have been detected?
As of June 2016 there have been 691 cases of travel-associated Zika infection in the U.S. Most of these were contracted when the patient was traveling in an area of active infection and 11 were sexually transmitted. To date, in spite of the fact that the Aedes aegypti mosquito has been reported in several states, including California, Arizona, New Mexico, Texas, Louisiana, Florida, and Hawaii, there have been NO reports of locally mosquito-borne cases in the U.S. However, it is recommended that everyone remove sources of standing water (empty flower pots, tires, trash bins, even bottle caps) from around their homes and use mosquito repellant when outdoors.
What are the current CDC recommendations regarding Zika virus and reproduction?
POSSIBLE EXPOSURE is defined by the CDC as travel to or residence in an area of active Zika virus transmission OR sex (vaginal intercourse, anal intercourse, or fellatio) without a condom with a man who traveled to or resided in an area of active transmission.
- For a woman with Zika virus disease OR for a woman or man with possible exposure to the virus but without clinical illness: Wait 8 weeks before attempting conception from time of symptom onset or from time of possible exposure. This is based on approximate incubation period and the longest period of time the virus has been identified in the system after onset of symptoms.
- For a man with Zika virus disease: Wait 6 months before using his sperm to attempt conception. This would be through intercourse, vaginal or intrauterine insemination of a partner, or insemination of partner or donor eggs through IVF. Virus can remain in semen much longer than in blood, as reports of sexual transmission up to 10 weeks after symptom onset have been reported.
Virus shedding in semen may be intermittent, in which case a man’s semen sample could test negative but he may still carry the virus and shed it in the future.
Is it possible to freeze sperm or eggs prior to travel to an area of active Zika transmission?
If a male is planning to travel to an area of the world with active Zika and does not wish to risk having to wait 6 months before trying to have a child upon his return, he has the option of freezing his sperm prior to his departure. This sperm can be used for intrauterine insemination of the female partner or for insemination of her eggs or donor eggs via IVF/ICSI. If the couple plan to transfer embryos to a gestational surrogate, male FDA screening would have to be completed prior to freezing the sperm. In the case of a single male or a male/male couple, once male FDA screening had been completed, the sperm could be frozen and used for insemination of donor eggs via IVF/ICSI, with planned transfer to a gestational surrogate.
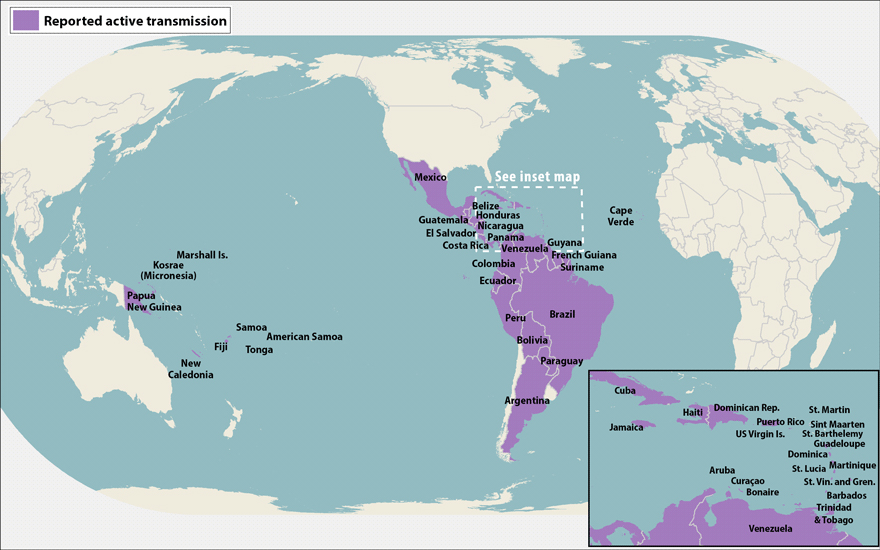
CDC Map of Zika Affected Countries 6/16
Likewise, a female could choose to freeze her eggs or embryos prior to travel to an area with active Zika infection, but if she becomes infected, her wait time prior to attempting to conceive with fresh eggs when she returns is only 8 weeks. Should she decide to freeze eggs or embryos prior to such travel with plan for embryo transfer to a gestational surrogate rather than to her uterus, she would undergo FDA screening prior to retrieval of her eggs.
How can a male minimize transmission of Zika to a partner after possible exposure to the virus, even when not planning conception?
A male with possible exposure to Zika could, upon return to the U.S., avoid unprotected intercourse with a female or male partner by using condoms for 8 weeks. If he is returning to a pregnant partner, they should completely avoid unprotected intercourse and fellatio (either through abstinence or consistent use of use of condoms) for the duration of the pregnancy.
What are the current FDA guidelines for Zika screening of donated gametes?
There is potential risk for transmission of Zika virus through donated tissues, including semen and oocytes. Virus has been detected in semen up to 10 weeks after the onset of symptoms even after it has been cleared from blood.
Effective March 2016, the FDA has recommended living donors of eggs or sperm be considered ineligible if they have any of the following risk factors:
- Medical diagnosis of Zika in the past 6 months.
- Residence in or travel to an area with active Zika transmission, within the past 6 months.
- Sex within the past 6 months with a male who is known to have either of the risk factors above.
8/2/16: Latest Zika Virus Updates
- The first female-to-male sexual transmission of Zika virus in the U.S. has been reported. On July 15, 2016, the New York City Department of Health announced the first case of a woman transmitting the Zika virus to a man via condom-less vaginal intercourse on the day she returned from a country with ongoing Zika transmission. The couple had not had oral or anal intercourse. The female had the onset of Zika symtoms including fever, fatigue, and rash the next day. Zika virus RNA was detected in her serum and urine. The male partner experienced onset of symptoms 6 days later and Zika virus was found in his urine. He had not traveled to a Zika prone area in the past 12 months, had not been bitten by a mosquito within a week before onset of symptoms, and had not had recent intercourse with any other partner. Therefore, it was concluded that the virus may have been transmitted to him via the woman’s vaginal fluids. Recent research has found the Zika virus in the vaginal fluid of infected females.
- The CDC has updated its recommendation that all pregnant women use barrier methods of contraception during sex or abstain from sex completely, with a partner who has traveled to an area with active Zika transmission, to now include female sex partners as well as male partners.
- French pharmaceutical company Sanofi has struck a deal with the U.S. Army to work on a Zika virus vaccine, which may be ready for testing on humans by October, 2016. An Austrian biotech company, Themis Bioscience is also working on a vaccine for Zika virus and stated it plans to start clinical trials in the next 12 months.
This blog is for informational purposes only as CDC recommendations will continue to change as more information is learned about the Zika virus. One should consult with one’s own physician for current information and recommendations.
For current updates on Zika virus, go to: www.cdc.gov/zika
Thank you to our guest writer Dr. Janice Andreyko for publishing this informative piece.




